What should you do when the most intense and transformative experience that is childbirth delivers trauma that is physical as well as emotional? ACC modelling suggests around 60% of the 47,000 maternal birth injuries that occur each year will now be covered under the new Maternal Birth Injury (and Other Matters) Amendment Act. But do the changes go far enough? Sasha Borissenko investigates.
Suffering high blood pressure, Edith* was induced at 38.6 weeks on the advice there would be little to worry about. It was everything but.
Despite swearing to her husband she didn’t want an epidural in the delivery room – even if she begged – an anaesthetist administered the procedure an hour later. Pushing for long periods even when the contractions had subsided proved unsuccessful.
The baby was at risk and so a doctor was called, leaving her with three options – forceps, ventouse (vacuum delivery), or emergency c-section. The doctor recommended forceps, so thinking it could cost her baby’s life, Edith said yes.
Naked and in front of a room full of people – there was an overlap in staff changing shifts – Edith gave birth on the second push. The doctor repaired a third-degree tear, explaining it would take some time to heal but she was lucky it wasn’t as bad as a fourth-degree tear; it was no big deal.
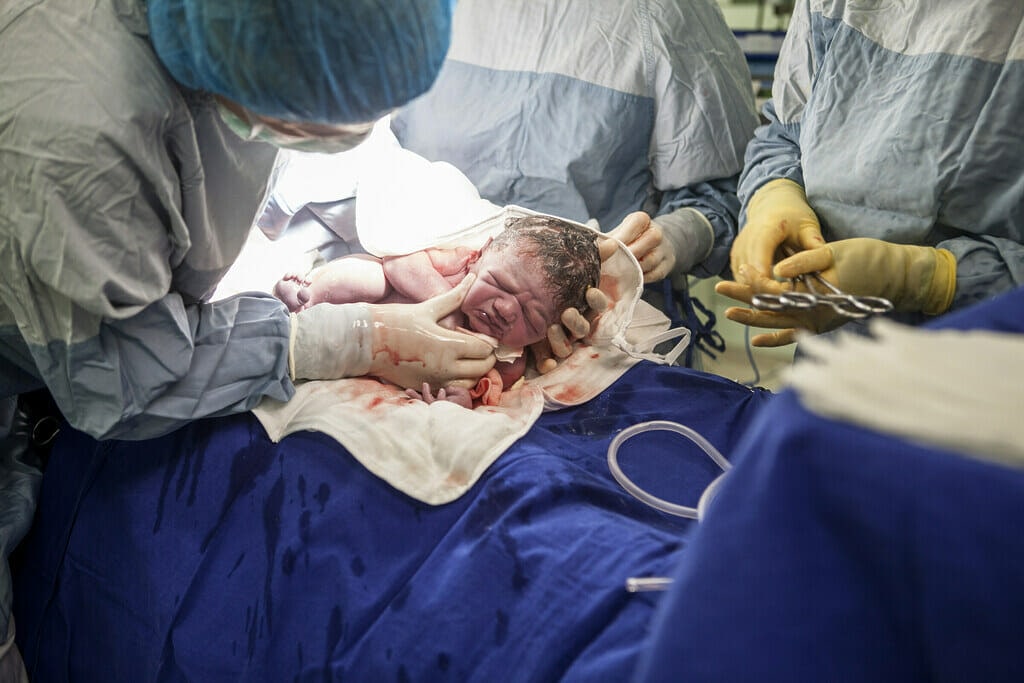
According to Accident Compensation Corporation (ACC) data, the most severe perineal trauma involves the anal sphincter, known as third and fourth degree tears or obstetric anal injuries – occuring in 2-3% of vaginal births. These rates are greater in first-time births (5.7%) and the rates are greater when vaginal births are assisted by instruments like vacuum or forceps (7.2%).
Research suggests women with a history of forceps-assisted vaginal delivery are twice as likely to suffer a prolapse. For Edith, nine weeks later something wasn’t right. The sense of heaviness meant she avoided walking – even around the house – for fear of her uterus or bladder falling out. She’d suffered a prolapse, prompting the need to have surgery.
On top of anal fissures, constantly needing to go to the toilet, caring for a newborn, and feeling the stigma associated with birth injuries, the trauma of the experience was too much.
“I felt overwhelmed by my birth experience, horrified it had gone the way it had, disgusted at myself for not just being grateful that my baby was safe and I felt embarrassed and so stupid to be feeling sad.”
Over time, Edith’s symptoms – psychological and physical – lessened. It was only when she gave birth to her second child – a vastly different and empowering experience – that she found her sense of power again.
Edith is one of three birthing people to have reported having a traumatic birth. Physical injury to the tissues between the vaginal opening and anus during childbirth affects around 85% of women who give birth vaginally. For people who have experienced a physical birth injury and mental trauma as a result of that injury are now covered under the Accident Compensation (Maternal Birth Injury and Other Matters) Amendment Act.
For people like Edith who suffered injuries prior to October 1 of this year, and those who sustain an injury not specifically listed in the legislation – including mental trauma in and of itself – it means they’ll have to bear the brunt of a stressed public health system or go out of pocket.
For many, the changes signify a culture-change shift for the better.
Dr Melissa Davidson is New Zealand’s only doctor specialising in pelvic health physiotherapy. She serves on the ACC expert advisory group and has trained physiotherapists for 32 years.

“A woman may have had ongoing pain for 30 years. It may have affected her relationship with her partner, you know, not wanting to ever have ‘that thing’ [a penis] near them because of the damage done during childbirth. We can teach them how to stretch or work with the scar tissue so that there’s no pain during sex. That’s now subsidised. It can be life altering for that woman.”
There are now no caps on the number of people needing access to clinical pathways or the number of treatments available, she says.
It’s also relieving pressure on the health system, she says. There are approximately 26 full-time equivalent physiotherapists covering a range of injuries in District Health Boards throughout the country. With close to 250 private pelvic health physiotherapists now eligible to take on ACC patients, it means wait times will drastically decrease. The legislation also allows pelvic health physiotherapists to diagnose injuries, which relieves the pressure on gynaecologist clinics.
Previously, women with birth injuries would have to wait or pay privately for support, now, ACC will even the playing field and enable women in whatever town they’re in to access physiotherapy, she says.
Caitlin Day of Unity Studios is a women’s pelvic health physiotherapist and clinical pilates instructor. Graduating in 2009, she never had aspirations to work with the All Blacks and her understanding of pelvic physiotherapy was limited by the one-hour lecture during her four year degree.

Working in a hospital, she saw volumes of women coming in with prolapses and incontinence issues and seeing the need for specialists, she took up a two-year post graduate degree in Melbourne. It was time intensive and costly but she’s never looked back.
“It’s really amazing to be able to help people with issues that are so intimate and taboo but through care it can make a massive difference to people’s lives.
“It’s not the nicest thing to have a vaginal assessment but it’s important for people to feel prepared – I see vaginas all day, everyday. And hopefully the media attention following the ACC changes will help to shift the stigma surrounding pelvic health.”
Day is hopeful the changes will lead to more of a focus on prevention.
“Some of these injuries are for life. If your pelvic floor doesn’t repair your body adjusts – there’s no surgical way of fixing it at this point. It means the woman is more at risk for prolapses later on in life and she’s more likely to suffer incontinence in her old age.”
“Even without tearing, the pelvic floor muscles and structures stretch about 2.5 times the resting length during a vaginal birth. You could argue there’s no way that the muscle can come back without intervention. You might not meet the criteria to qualify for ACC but we know things are likely to get worse as time goes on.”
Studies estimate 11% of women will require prolapse surgery before the age of 30. One study dating back to 2001 found the direct costs of pelvic surgeries were over USD$1billion a year.
In countries such as France and other parts of Europe for example, women are eligible for free pelvic physiotherapy before and after birth. The UK has followed suit, rolling out a pilot for free pelvic physiotherapy following the 2020 Cumberland Inquiry into mesh treatment.
Pelvic physiotherapy has been shown to decrease leaking urine, pain, and prolapse when implemented effectively. It can also help reduce the risk of tearing if performed during pregnancy.
ACC changes – close but no cigar
For John Miller Law lawyers Brittany Peck and Maria Bagnall, the ACC changes don’t address the fundamental issues at the heart of ACC.
Bagnall and Peck were one of 815 people to write submissions during the legislation’s consultation process. For one, it’s not retrospective, meaning anyone who gave birth prior to October 1 isn’t covered.
ACC Minister Carmel Sepuloni says the Act is designed to capture current levy and tax-payers who fund injuries that happen now. It also meets Cabinet’s Legislation Guidelines, which state that legislation should have prospective and not retrospective effect, except in specific circumstances. Finally, retrospective changes come with larger costs.

“If we make one change retrospective, it means any future changes would have to be done that way as well. This would potentially discourage future Governments from making changes.”
Bagnall says the prescriptive and restricted approach is piecemeal.
”Women are more likely to suffer injuries that are not recognised or are accepted as easily because our current scheme is imbued with these old fashioned ideas about what and who does work.”
Peck says it comes back to the analogy that if you sprain your leg on the rugby field, you’re instantly covered with no questions asked. But traditionally people seeking cover for birth injuries, secondary trauma or gradual injuries among female-dominated workforces have been left out in the cold.
In fact, there is a NZD$1b annual pay-out difference between men and women from ACC. While the costs of the new legislation are estimated to be around NZD$25m annually, the costs to women with significant existing untreated injuries have never been recorded.








